Stressed About Hysterectomy Risks? What Every Woman Must Know
Hysterectomy risks and complications concern every woman scheduled for a hysterectomy.

Although a hysterectomy is a procedure that can save a woman’s life with certain medical conditions, it is a procedure that comes with certain risks.
Removing the uterus is one of the most common surgeries performed today, and less than ten percent of hysterectomy patients experience minor or major complications.
This blog is reader-supported. When you buy through a link on our site, we earn a commission at no extra cost to you. Read more
Knowing about the potential hysterectomy risks and complications will help you make a better decision and have a positive post-surgery experience.
Here is an overview of hysterectomy risks and complications:
Bleeding
One of the major risks of the surgery is excessive bleeding. This can occur on entry during laparoscopic surgery. Entering into the abdomen laparoscopically is associated with a 0.1 percent risk of damage to the blood vessels like the vena cava or aorta. The amount of blood loss can vary and depends upon various factors. A small to moderate amount of blood loss is normal. However, a blood transfusion is necessary in case of excessive bleeding, and open surgery may be unavoidable.
Moderate or light vaginal bleeding may continue throughout the recovery period. Reasons women may experience abnormal bleeding from the vagina include:
- Vaginal vault infection
- Excessive use of heat to tissue during surgery
- The material or technique used to close the vaginal vault
- Resuming strenuous physical activity too soon
Infection
Women undergoing pelvic surgery should get prophylactic antibiotics as the risk of infection during and after the surgery is high. Such an infection can occur at the site of the incision days after the surgery is over. The first days after the operation, they regularly measure the temperature since fever is one of the first signs of postoperative infection.
Signs of infection in a surgical incision include:
- increased pain
- discharge from the wound
- the area around the incision is warm and red
- the area is tender to the touch
Sometimes, infections develop after discharge from the hospital. Vaginal or skin incisions can open and get infected and may need re-admission to the hospital. If you notice any of these symptoms, contact your healthcare provider immediately.
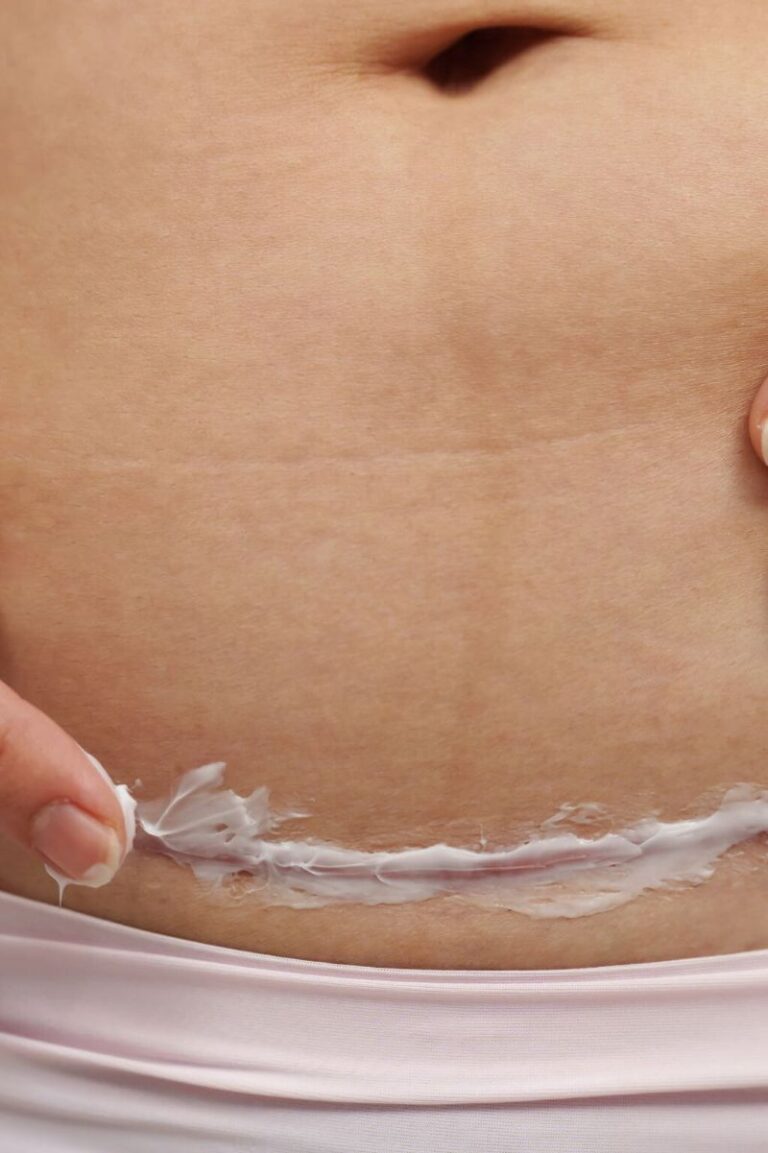
Read also: Managing Hysterectomy Scar Tissue: 10 Techniques and Treatments
Complications of anesthesia
With modern medication advancements and monitoring technology, the safety measures for inducing anesthesia have increased multiple-fold over the last few years. But, anesthesia is a risk of hysterectomy that one has to consider as it can sometimes lead to serious complications. Some of the complications of anesthesia include stroke, aspiration, heart attack, lung infections,
Women at a higher risk of complications from anesthesia are women:
- who smoke a lot
- with higher body weight
- with a heart or lung condition
It is important the anesthesiologist learns about existing respiratory problems, allergies, and heart conditions.

Damage to surrounding organs
Hysterectomy can be traumatic for surrounding organs. During the surgery, there is a risk of damage to the urinary bladder, ureters, and bowels. Damage to any of these organs needs immediate repair surgery. At times, the symptoms of urethral, bladder, or bowel injury do not become obvious until several days after the surgery.
If you develop the following symptoms, then consult your surgeon immediately.
- Abdominal distension
- Fever
- Nausea and vomiting
- Back pain
The risk of complications with a laparoscopic (L/S) hysterectomy is not notably higher than with an abdominal hysterectomy. L/S hysterectomies take longer, which means more anesthesia, but recovery rates are faster. The choice of type of hysterectomy is generally based on the surgeon’s experience and the size of the uterus.
The greatest risk of injury during a laparoscopic hysterectomy is when there are adhesions. When adhesions are present, an open procedure may be a safer choice.
Small bowel obstruction
During the recovery phase, your small bowels can become obstructed or twisted, obstructing the normal flow of its contents. The number one cause of small bowel obstruction after a hysterectomy is adhesions. A potentially life-threatening complication that is more common after abdominal hysterectomy. It can happen days after surgery but can also occur years later.
The first signs of intestinal obstruction are:
- distended abdomen
- the inability to pass gas
- nausea and vomiting
- abdominal tenderness
- severe cramping pain
Often, surgery is necessary to remove the obstruction and clear the passage.
Pulmonary embolism
After every major surgical procedure, the patient is at risk of developing a blood clot. This is because of immobility during and after the operation. They may develop in the deep calf veins, causing pain, warmth, and swelling. A blood clot can break off and move upward to the heart, lungs, or brain when not treated. This is a life-threatening situation as it deprives these organs of oxygen.
When it blocks the circulation in the lungs, it will cause:
- sharp pain when breathing
- shortness of breath
- increased heart rate
- fever
- spitting up blood
To prevent blood clot formation, nurses will urge you to get up and move around immediately after the operation.

How can you lower your risks?
We did not round up this list of hysterectomy risks to frighten you but to give you an understanding of what will increase your chances of a successful outcome.
What you can do:
- When you are scheduled for surgery, you should stop smoking. Most anesthesiologists will look concerned when they hear a woman is a heavy smoker, as it may increase her risk of breathing problems during and after surgery.
What you need to know about the risk of cigarette smoke on anesthesia.
- Many doctors will recommend heavier women lose some weight before surgery. Surgery time can take longer for heavier women, who also experience more complications after surgery than nonobese women. A healthy weight also helps speed up recovery after a hysterectomy. And not to forget, losing weight will be a lot easier before than after the hysterectomy.
- Restrict your daily strenuous activities for the first weeks following surgery. Avoid bending, heavy lifting, and straining. These activities not only increase swelling but also put pressure on the wound, and it can start bleeding.
If you like to read more about hysterectomy risks and statistics, you can find a very detailed list at hersfoundation.com.
Reviewed by: Kimberly Langdon M.D. (OB/GYN)
Date reviewed: 18/3/2019





Thank you for your story. I am 57 have a very large ovarian cyst on my left ovary. If it is cancerous, which it currently appears not, they will do a hysterectomy. If not…..I have to decide if I want to do it because they are there. I have read many old posts and am glad to see yours from this past year.
How are you doing now nearly a year out? Have you had any spine issues? Any incontinence issues?
I have many friends who have had hysterectomies and glad they did. Others only had ovaries removed. I am concerned about the bladder and bowel issues from the space left if everything is removed. These bladder issues scare me. I am seeing a female GYN for additional pre-op consultation for pros and cons. The surgeon is a well respected man.
The more I read, seems the more confused I get.
Cyndi Johnson
California
Part of me wants to get rid of the parts and not worry of future cancer issues. This whole health care coverage thing could be problematic for future treatment for me as I am self-employed.
Wow – thank you for your post!!! This is what I” m dealing with daily NOW at 44 and today I met with my Gyno to discuss removing everything as I’ve tried all my options and this is the last thing. Reading your post makes me feel like I’m not alone – I have the extreme fatigue – the “depression” but kept saying I” not depressed – I still go do things still enjoy then get zapped and out of life for a couple of days!!! You don’t know how much your post means or how timely it was I found it and this site ! Thank you!
Hi my name’s Alechia Edinbourgh,and I had my Hysterectomy 11/18/2016. I was doing just fine with post op after care at home. I went back for my follow up exam,and everything was working fine. I returned back to work right after my follow up exam. After the 3rd day,i started having pain between my breast. On the scale of 1to10,it was a 3. I knew that I shouldn’t be hurting like this. So I went to the emergency room. They ran test on me to find out why I was hurting. Come to find out,i had a blood clot in my lower left lung. The pain was in the middle of my chest. I couldn’t understand why it would be hurting in the center of my chest when the clot was in my lower left lung. Reverse pain. Emergency doctor placed me on syringe blood thinners and pill form blood thinners. I have been taking this medication for the past 4days. I’m bleeding through my pads. I’m waiting on the doctor’s response. Please pray that I don’t bleed to death.